Endometriosis Pain Relief and Surgery: A Complete Guide to Treatment
Facts:
- Endometriosis affects an estimated 1 in 10 women worldwide.
- Minimally invasive surgery is the leading trend for endometriosis treatment.
Navigating the Path to Endometriosis Pain Relief
Endometriosis is a complex and often debilitating condition characterized by the growth of tissue similar to the uterine lining outside the uterus. The primary symptom is severe, often unmanageable pain, which can manifest as excruciating periods, pain during intercourse, and most notably, `chronic pelvic pain`. Finding an effective `endometriosis treatment` plan is crucial for restoring quality of life. This guide delves into the primary avenues for managing this condition: comprehensive pain relief strategies and the role of advanced surgical interventions, providing a clear roadmap for patients seeking solace from persistent `endometriosis symptoms`.
Understanding Endometriosis Symptoms and Diagnosis
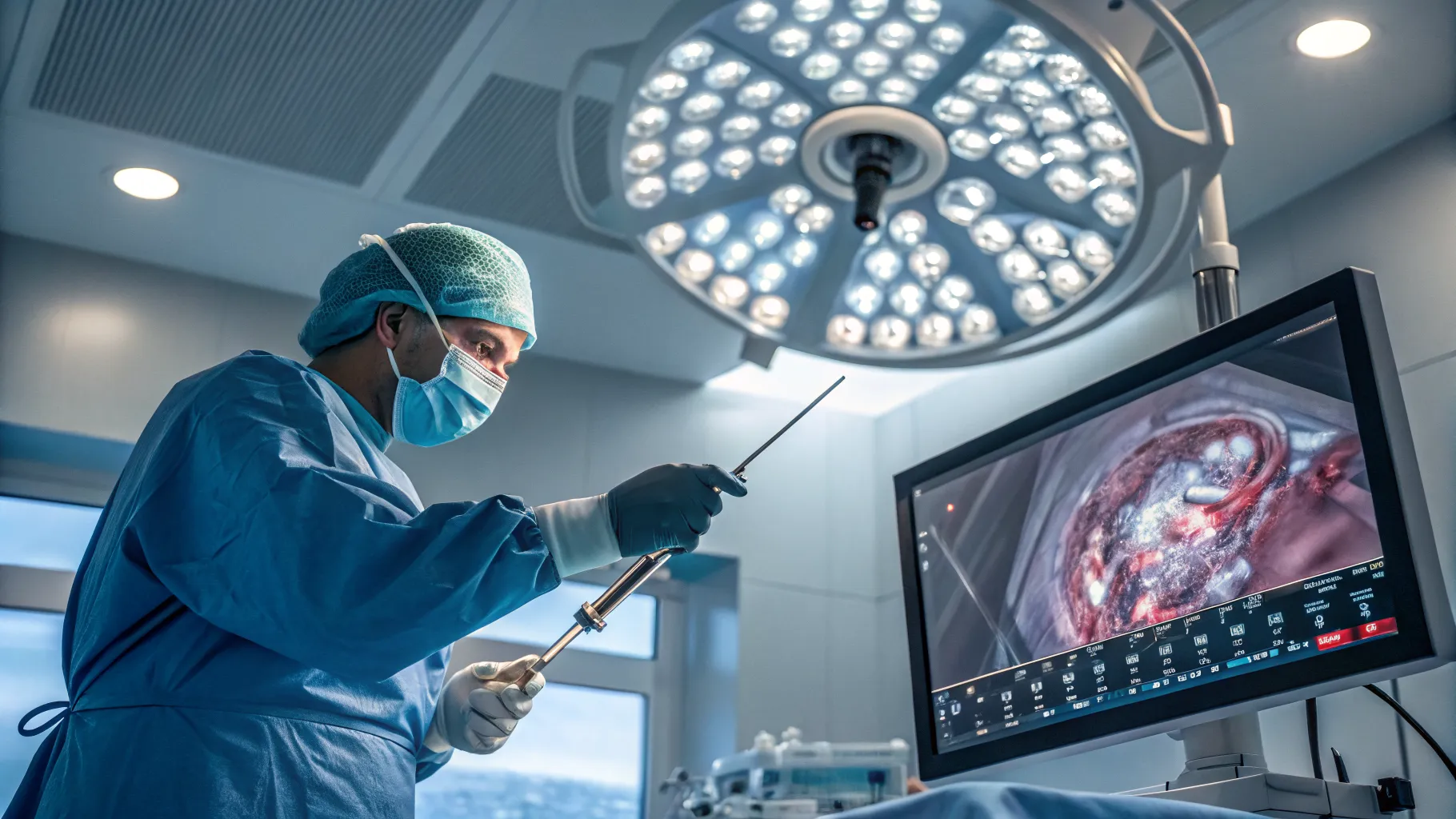
Recognizing the wide array of `endometriosis symptoms` is the first step toward a diagnosis and effective management. While intense menstrual cramps and `chronic pelvic pain` are hallmark signs, the condition can also cause fatigue, bloating, nausea, and pain with urination or bowel movements, particularly during menstruation. The severity of symptoms does not always correlate with the extent of the disease. A definitive diagnosis often requires a surgical procedure. While imaging like ultrasound or MRI can suggest the presence of endometriomas (cysts), the gold standard for diagnosis is `laparoscopic surgery`. This minimally invasive procedure allows a surgeon to visually confirm the presence of endometrial implants and take a biopsy for confirmation, providing a clear basis for a tailored `endometriosis treatment` plan.
Non-Surgical Approaches to Endometriosis Pain Management
Before considering surgery, many individuals explore non-surgical options to manage their `endometriosis symptoms`. The cornerstone of medical management is often `hormonal therapy`. By suppressing or regulating the menstrual cycle, these treatments can slow the growth of endometrial tissue and reduce inflammation, thereby alleviating pain. Options include combined oral contraceptives, progestin-only pills, GnRH agonists, and hormonal IUDs. Each type of `hormonal therapy` has its own profile of benefits and side effects, making a discussion with a healthcare provider essential. Alongside hormonal treatments, nonsteroidal anti-inflammatory drugs (NSAIDs) can help manage acute pain. Complementary therapies such as pelvic floor physical therapy, dietary changes, and acupuncture are also gaining recognition for their role in managing `chronic pelvic pain` associated with endometriosis.
The Role of Surgical Intervention in Endometriosis Treatment
When medical management fails to provide adequate relief or when fertility is a concern, surgery becomes a primary `endometriosis treatment` option. The most common and effective procedure is `laparoscopic surgery`, which involves making small incisions in the abdomen to insert a camera and specialized instruments. The goal is to excise (cut out) or ablate (destroy) all visible endometrial implants, adhesions, and cysts. Excision is often preferred by specialists as it completely removes the lesion and allows for pathological confirmation, potentially leading to lower recurrence rates compared to ablation. A skilled surgeon can meticulously remove the disease while preserving pelvic organs, which is critical for future fertility. For severe cases where other treatments have failed and childbearing is complete, a hysterectomy with removal of the ovaries may be considered, but this is typically a last-resort `endometriosis treatment`.
Comparing Medical vs. Surgical Endometriosis Treatment
Choosing between medical and surgical `endometriosis treatment` involves a careful consideration of goals, symptom severity, and life stage. `Hormonal therapy` is less invasive and can be highly effective for managing `chronic pelvic pain`, but it does not remove existing lesions and symptoms often return once treatment is stopped. It is not a solution for those actively trying to conceive. In contrast, `laparoscopic surgery` aims to physically remove the source of the pain and can improve fertility rates. However, surgery carries inherent risks and does not guarantee a permanent cure, as endometriosis can recur. Often, the most effective long-term strategy involves a combination of both: `laparoscopic surgery` to remove the bulk of the disease, followed by `hormonal therapy` to suppress the growth of any microscopic residual tissue and prevent recurrence. This integrated approach addresses both the anatomical disease and the underlying hormonal drivers.
Actionable Steps for Managing Your Condition
Taking a proactive role in your health is vital for managing endometriosis. Here are actionable steps you can take:
- Keep a Detailed Symptom Journal: Track your pain levels, triggers, and the effectiveness of treatments. This data is invaluable for your doctor to understand your specific `endometriosis symptoms` and adjust your care plan.
- Seek an Endometriosis Specialist: General gynecologists may have limited experience. A specialist who frequently performs `laparoscopic surgery` for endometriosis will have the advanced skills needed for complex cases.
- Explore Pelvic Floor Physical Therapy: `Chronic pelvic pain` often leads to muscle tension and dysfunction. A specialized physical therapist can help release tension, improve muscle function, and significantly reduce pain.
- Build a Strong Support System: Connect with support groups online or in person. Sharing experiences with others who understand the challenges of endometriosis can be incredibly empowering and reduce feelings of isolation.
- Discuss Long-Term Goals: Have open conversations with your doctor about your long-term `endometriosis treatment` goals, including pain management, career impact, and family planning, to ensure your plan aligns with your life priorities.
Frequently Asked Questions
Is laparoscopic surgery a permanent cure for endometriosis?
While `laparoscopic surgery` is highly effective at removing existing endometrial lesions and providing significant pain relief, it is not always a permanent cure. Endometriosis can recur in some individuals over time. Post-operative management, often including `hormonal therapy`, is frequently recommended to reduce the risk of recurrence and manage any residual `endometriosis symptoms`.
How effective is hormonal therapy for managing chronic pelvic pain?
`Hormonal therapy` is often a first-line `endometriosis treatment` for `chronic pelvic pain` and can be very effective for many patients. By suppressing the menstrual cycle, it reduces the inflammation and growth of endometrial tissue. However, its effectiveness varies from person to person, and it may take trying a few different options to find the one that works best for you.
Can I get pregnant after undergoing endometriosis treatment?
Yes, many people go on to have successful pregnancies after `endometriosis treatment`. For those with fertility issues caused by endometriosis, `laparoscopic surgery` can improve chances of conception by removing scar tissue and restoring normal pelvic anatomy. It is crucial to discuss fertility goals with your doctor to create a treatment plan that supports them.
References
- Journal of Minimally Invasive Gynecology
- American College of Obstetricians and Gynecologists (ACOG)
- World Endometriosis Society Clinical Practice Guidelines
- Human Reproduction Update Journal
Authored by 24Trendz team